The most comprehensive guide to headache
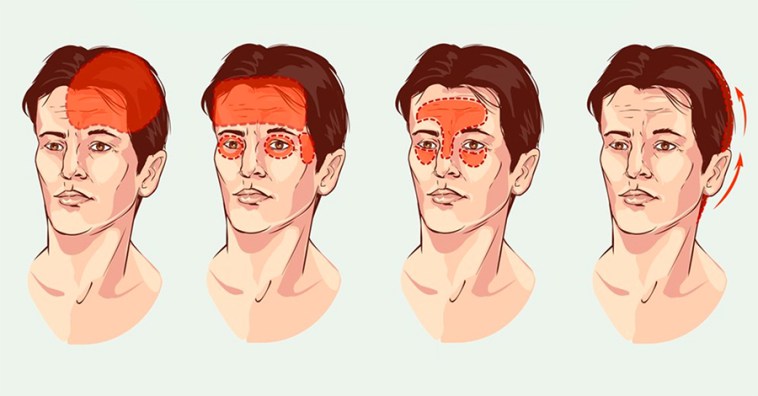
Anton Loboda, an anesthesiologist, resuscitator, specializing in getting rid of pain, told everyone about the pain and answered a number of questions. We publish his guide for pain with permission of the author and from his first person.
On the medical profession: pain management ("work with pain")
It's worth mentioning that I went to medicine precisely with the goal of getting people out of pain, anesthesiologist-resuscitator became from the same considerations and now I'm leaving for a separately developing specialty - a pain management specialist for the same reason.
Why a specialist in pain? And so all the experts know everything. The problem is that the expert to whom come with pain, will only look at his own and if he does not find one, then sends him further down the list. For example: there is a person's pain in the chest, he goes to the cardiologist, he refers to the pulmonologist, the one to the neurologist and this can continue or until the chronic pain or self-passing. And the patient remains without a diagnosis, respectively, without recommendations for prevention and, if necessary, treatment of pain when they return.
A specialist in pain, assesses pain, finds a source and then, if necessary, sends to the specialists already diagnosed with this while trying to maximize anesthetize and give recommendations for anesthesia.
What is pain?
The pain is different. There is the concept of acute pain, it is instant and intense. There is the concept of chronic pain, and often there is no longer a substratum for pain, everything has already healed and gone, but there is pain and then this pain is not intense, but more exhausting.
In general, pain is the body's response to a stimulus with a subjective emotional color. This is really an evolutionarily verified mechanism, which is protective: damaged - do not load. Another issue: the mechanisms of damage are different and the structures are damaged differently and the pain from these structures is perceived in different ways. And sometimes everything will heal, but the pain is still there.
Scale of pain
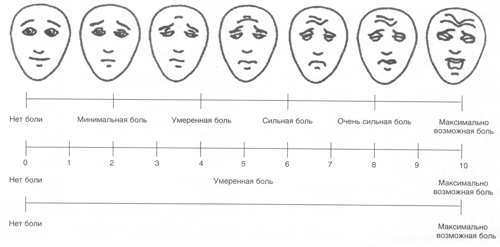
A person comes to you with 10 out of 10 points on a visual analog scale, and leaves with 2 out of 10. A very clear result: out of intolerable pain there remained a low background pain.
After local injection therapy, one can understand whether or not it got there, whether the punctured structure is the source of pain and / or how much (if any) contributes to its contribution.
Headache and myths about her
About the headache you can speak endlessly, it is individual from the beginning of its formation to the trigger moments, because of which it arises. The head really hurts in a special way and this characteristic the patient can not usually clearly state. It hurts something, somehow, somewhere, as if. While I describe three types of pain, the most frequent, and then I will add extravagant cases. Just scatter a couple of established myths!
Myth: a headache is a sign of high blood pressure.
The truth is only in the case of a lenticular current (figures above 180/120 mm Hg). In terms of migraine, so in general, increased blood pressure is the prevention of seizures or their cupping.
First, the pain itself in part stimulates the sympathoadrenal system, which gives rise to arterial pressure. Secondly, the increase in pressure is psychologically increased. Thirdly, there is the concept of the error of measuring pressure: an incorrect technique for measuring pressure, a clogged-up tonometer, have not prepared for measurement.
Especially the last moment, when a couple of times a person comes to me from the office after 3 mugs of double espresso, 2 cigarettes, a sleepless night and bring it to me from some super important meeting. And here he in a panic requires a pill, I give him a pill, not only from pressure, but calming and I ask 10 minutes in a darkened room to lie down to count his breaths. And, oh miracle, the pressure is normal.
There was a study in the field of sports medicine, where runners, weightlifters and swimmers measured the pressure during physical exertion. An untrained person would immediately say that a person has a hypertensive crisis and urgently needs pills, but they did not die and the pressure at them at the end of the loads returned to normal. The mechanism of increasing pressure under stress and physical exertion is approximately the same. And the head, by the way, did not start to ache from the pressure increase.
Myth: no-shpa will relieve the headache.
This is not true. If no-shpa helps, then the effect of placebo with the same headaches of tension is not canceled. With them, you can accept almost anything, anything, and this will work, but most likely because you really want it to work.
There are 4 main types of headache:

Further about them in more detail: how to define and treat them.
Headache of intense type
We must be honest and say that it is not known what exactly it hurts: research has been underway since the mid-1980s. At first it was believed that the muscular hypertension of the occipital region and neck gives pain, checked - no, the muscles are normal. However, we decided to leave the term "headache of a strained type" or "tension headache". What we managed to find out: pain is clearly associated with stress. Accordingly, the problem is not only outside, but also inside, or rather somewhere in the area of the hypocampus.
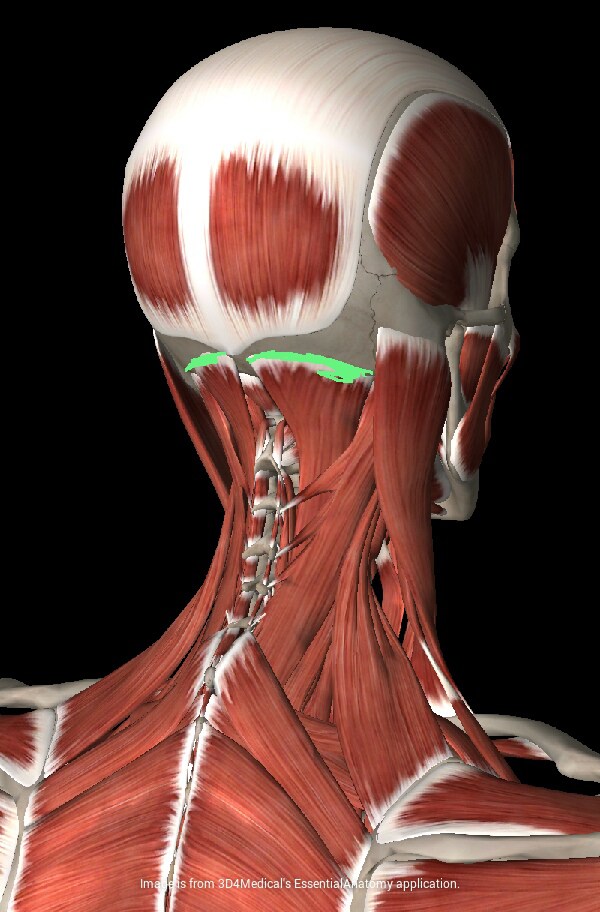
In green, the doctor noted places of common soreness with enthesopathies.
He often talks about enthesopathy, especially in the area of the base of the skull - an interesting thing. Enteases are the areas of attachment of the muscles to the periosteum. These points are very intensively innervated (that is, they have a lot of nerve endings) and, consequently, minimal traumatization of this area causes pain.
An analogue of the inflammatory process that follows traumatization can be sustained for a long time due to the fact that we are active people and willy-nilly we twist and twist our head and give tension to the already traumatized area. This I often see in practice: severe patients or with severe headaches I do injections of painkillers in the area of the occipital muscles and everything goes perfectly.
Diagnosis of severe type of headache
In the United States, both for tension headaches and migraines (but migraine is a separate topic, we'll discuss it in more detail below) have a system of criteria.
For a tension headache, two criteria should be present from the following:
- Pain pressing or squeezing, not pulsating;
- Occipital parietal / occipullo-frontal localization;
- Bilateral (bilateral) medium or low intensity (according to visual analog pain scale - this is usually 1-5 points);
- Does not increase with physical activity.
It is worth noting that this pain does not interfere with life, and often when you communicate with such a patient, you start telling him something, showing, distracting in every possible way - the pain disappears, but appears when the distraction stops. This once again confirms that something in the brain is developing and supporting it.
Tension headache is also divided into paroxysmal (acute) and chronic. The attack lasts from 30 minutes to 7 days. At chronic: not less than 15 days in a month not less than 6 months in succession. It should be noted that this pain can be background and subjective, people do not even perceive as a headache, but it is still a headache.
Treatment of a headache of intense type
First line:
- NSAIDs (non-steroidal anti-inflammatory drugs) such as aspirin, ibuprofen (nurofen), ketoprofen (ketonal), indomethacin and other or selective blockers of COX-2 and coxibs (celecoxib, etheroxib);
- Antipyretics / analgesics such as metamizole (analgin) or paracetamol (usual dose 1 gram).
I prefer to initially prescribe paracetamol, it well helps in a dose of 1 gram. Ketorol very well anesthetizes, but I never appoint it and in every possible way it or him aside because of gastotoxicity: can cause ulcers of a stomach and a duodenal gut.
Paracetamol is the safest drug at the moment, 1 gram 4 times a day - is considered a safe dose. Instead of ibuprofen, I would recommend coxibs, those on the stomach act to a lesser extent, but the kidneys also act, however, you can also take for a long time with the protection of the stomach (take after eating, diet + proton pump blockers) - judge by the patients who do this They accept for life.
In general, NSAIDs will soon come to naught when there will be generics of celecoxib. (Original - a little expensive).
Second line:
- More powerful painkillers in combinations paracetamol / codeine, paracetamol / tramadol.
Third line:
- Add antidepressants, but this is for chronic headaches of tension.
In our country, a very strange and extremely wrong attitude towards antidepressants. Just recently returned from Austria with training in the school of pain management, where the German pain specialist said that 100% of patients undergo a psychiatric examination as part of the monitoring of depression.
Pain itself is a vile thing, except for masochists, no one especially does not like it, but here it is for a long time, and even for good, it climbs into your life. Whether pain provokes and supports depression, or initially hidden depression provokes and supports pain. Communication has been proven, it exists and something must be done with it. In this context, the appointment of antidepressants is justified and necessary.
The task of antidepressants is to reduce the number of seizures in combination therapy (I always emphasize this for one pill you will not take away complex pain), ideally to zero. And I immediately explain: we do not treat antidepressants with depression as such, we remove the depressive component of chronic pain. Often patients refuse to take antidepressants, they say why they tell me, I'm not depressive. It is necessary to explain that depression is a serious disease that has different severity. One person walks with depression in a window after a couple of years of the disease, and someone with a mild depression deceives himself for years without even thinking that the daily negative that allegedly falls on him is the manifestation of this very mild form of depression, this without pain.
And if with pain, then the life of an ordinary person and the life of a person with chronic pain, or rather a person who did not have pain and then it arose and was chronicled - these are two different lives. For example, you often question the patient, about his past - to the pain and he talks about himself as a different person: "I traveled / worked / loved to do (insert missed), but now I can not because of the pain." And this is one of the sources of the depressive component.
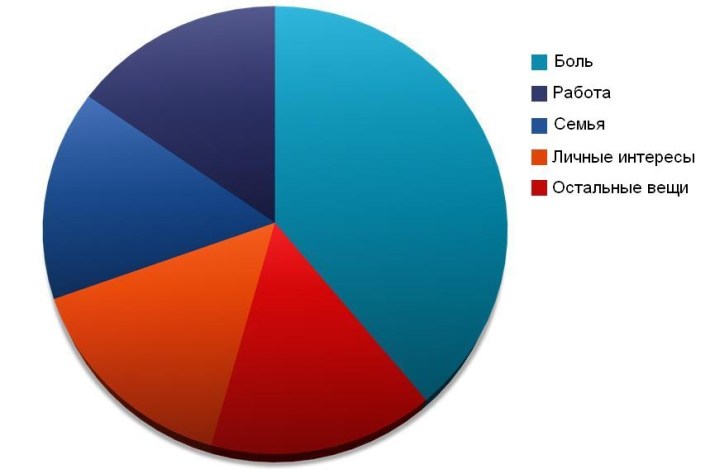
Ideally, of course, you need an examination of a psychiatrist in order to professionally confirm the depressive component and how much it is expressed, which in patients with chronic pain is close to 100%.
It is worth noting that with an uncontrolled constant intake of medications, a drug-induced headache may develop. That is, the pain associated no longer with the original problem of a headache, but with the direct taking of an anesthetic. Usually this develops after 3 months of systemic administration and it is very difficult to distinguish the tension headache or migraine from a medically induced headache.
That this was not a simple rule: no more than two drugs per day no more than twice a week.
Tablets - this is of course good, but we must understand that the headache is not the cause but the effect. So I recommend to change a way of life:
- Regular physical activity / sports (if you do not do it in the gym, at least just go for at least 2 hours a day, do not stand on the escalator, but go.) Do not wait for the elevator, but go up the stairs. Further);
- Refusal from smoking and a lot of coffee;
- Normal way of life: sleep mode (too much sleep - bad, too little - bad, 6-9 hours - normal), regular meals (usually often fractional 4-5 times a day in small portions, hunger is a pretty serious stress provoker) well and so on.
- Various meditation techniques, cognitive-behavioral techniques, consultation of a psychiatrist and psychotherapist to select and change attitudes towards stress and increase stress resistance. After all, it is important not only that we experience pain, it is important how we perceive it and how much we are able to control it, and not it us.
Also, the cause of pain may be calcium deficiency. Sometimes a patient comes in, you look at the lower braids of the muscle, and there they are tense and painful on both sides. This is often the case with calcium deficiency tetany. All around it is said that it's necessary to drink calcium, but few people know that calcium is not absorbed from the intestine if there is a deficiency of vitamin D. Accordingly, against the background of calcium deficiency, a persistent muscle hypertonia is formed, which gives not only a headache, but also painful sensations in many Parts of the body. Along with muscular pain, there are limb / face cramps, a feeling of coma in the goal, which can not be swallowed or shaken when swallowed (as a result of spasm of the esophagus), these are the main symptoms. Analgesics and relaxing muscles of the pill in this case will not help or help, but not for long and not until the end. It is necessary to restore vitamin D.
Migraine: what is it, the kinds of how to treat

The oldest disease. From history I will say that the name was born because of a perverted translation from the Greek word hemkrania ("pain on one side of the head") into Latin in the form of hemigranea and then into the French migrane.
For people suffering from migraine, I officially declare: at the moment, migraine is not treated . This is a hereditary or acquired thing that is characterized by brain dysfunction. No, this does not mean that there is a tumor or some other pathology. This means that, unlike other people, your brain reacts a little to some of the headache-provoking factors.
This begs the simple conclusion: find provoking factors and avoid them, take control. This is one of those diseases (as in many chronic diseases), where the doctor has a very small effect of exposure. We as doctors give you tools, and you must work with the disease yourself, for you we will not do it.
What is the cause of migraine? As in the tension headache: unknown. It used to be thought that the problem is in the blood flow and spasm of vessels or their expansion. Have checked up a blood flow on an attack - it's OK. Now the concept is not vascular, but neurogenic-vascular. Primarily, for some unknown reason, neurogenic processes occur, which lead to sterile inflammation in the brain with secondary changes in cerebral blood flow.
I singled out the word "change", since this is not a violation, it is an option of dysfunction. Everything works, but it works a little differently. The light bulb does not blink, it burns, but not as brightly as before, and then flares up again.
Genetics works here by about 70%. A huge negative factor: if a person is neurotic, with excessive susceptibility and mental instability, cognitive-behavioral disorders, acute reactions to stress, panic attacks and so on, anxious-hypochondriacs, so to speak.
Here is what the international headache company writes on the diagnosis of migraine: the first: there must be at least 5 headaches lasting from 4 to 72 hours, also these headaches should have two signs from the following:
- Unilateral (one-sided) localization;
- Pulsating nature of pain;
- Pain from medium intensity to very severe (usually 5 to 9-10 on a pain scale)
During a headache, there should also be at least one of these signs:
- Nausea or vomiting;
- Photophobia or phonophobia (hostility / phobia of light or loud noises);
And in the end, everything presented above should not interfere with other diseases at the time of the patient's examination.
Officially diagnosed migraine variants:
- Migraine without an aura (a common migraine);
- Possible migraine without an aura;
- Migraine with aura (classical migraine);
- Possible migraine with aura;
- Chronic migraine;
- Chronic migraine associated with excessive use of painkillers;
- Children's periodic syndromes, which may be precursors or associated with migraine;
- A migraine disorder that does not fulfill the criteria.
A few words about migraine with aura and aura. By "aura" is meant sensory, motor and visual phenomena, temporary (from 20 to 60 minutes). There are individually, are in combination. The most frequent: a visual phenomenon, by the type of scotoma - it is the fall of the vision with zigzag boundaries, which eventually shifts to the periphery.
Here is a variant of scotoma ...

Treatment of migraine
Here everything is complicated and individual, as well as with tension pain. The difference is that this is a dysfunctional sore and, accordingly, there are drugs that treat pain (abortifacients), but there are those who are preventing its development (preventive).
Usually, if there is vomiting, then start with it: give antiemetics (antiemetic), then they also give NSAIDs, but in the highest effective dose, then, if it does not help, tryptane is added.
For the prevention of very different drugs and antiepileptic drugs and antidepressants, and drugs for reducing blood pressure, such as beta blockers, and calcium channel blockers, but not for the purpose of reducing blood pressure, but with the goal of preventing migraine. Recommend medicines is stupid, because everything is very individual: one person, helps, the other is not and vice versa. The most important thing is to understand what are provocateurs of migraine development and minimize contact with them, or always be ready to have abortifacients.
It is important to keep a diary of migraine: when the head fell ill, how, against what, what took, helped / did not help and how much? Step by step in yourself to understand and understand what is right, and what is wrong, what you need and do not need for you personally. The doctor here only arranges the beacons and points the way, but everyone must go by himself.
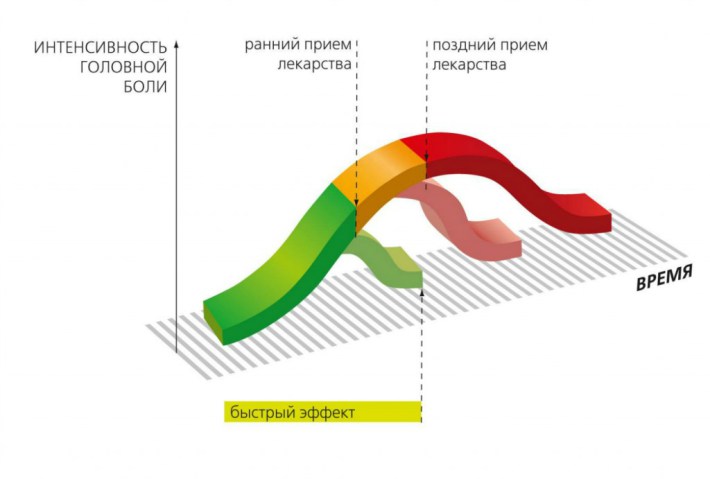 Bikyu Do not wait for the development of pain - the sooner you take the medicine, the better.
Bikyu Do not wait for the development of pain - the sooner you take the medicine, the better.
Just want to say one important point with migraines: do not wait for the development of pain. As soon as you understand that here it begins or has come, immediately immediately drink painkillers. The sooner you start, the better the effect.
Cluster headaches
Cluster headaches - severe headaches usually behind the eye, above the eye or in the temple lasting from 15 to 180 minutes from 1 time to 8 per day. Always 10 of 10 points on the scale of pain. Usually with them there is lacrimation, redness of the conjunctiva, runny nose, lowering of the upper eyelid or its edema, all on the same side of the pain.
The mechanism of development is not fully known. The genetic factor and the development of nonspecific inflammation in the cavernous sinus and upper eye vein are expected and the development of pain is somehow connected with the trigeminal-hypothalamic pathway. There are also trigger factors contributing to the occurrence: alcohol, nitroglycerin, relaxation / tension, histamine, large heights and flashing light.
In the form of an episodic and chronic. Episodic is the association of cluster pains in periods, that is, respectively, 2 cluster periods from 7 days to a year, separated by 1 month without pain. Chronic - this is when the painless period is less than a month.
It is also worth mentioning about neuroimaging, such pains are secondary, and MRI shows structural damage to the brain. So I recommend to all patients with cluster pain to do an MRI of the brain.
Very good oxygen helps, 10-12 liters per minute. It often happens that I give a breath, and after 15 minutes everything passes. If not very helpful, I add triptans, somotryptan for example. Triptans are good, but they can not be used often and still there are contraindications - cardiovascular sores, pregnancy. There is abortive therapy aimed not at preventing attacks, but rather at reducing the frequency of seizures. I read about lithium drugs and verapamil.
It also helps avoiding triggers - anything that causes pain. There is no provocation, no headache.
Synovial facial and headache
It also includes a rhinogenic headache . It's about you, always sniffing allergic nose, about you sinusitis with sore sinuses. Yes, headaches accompany sinusitis, and not just accompany, and sometimes are their first sign. Particularly weak, sluggish.
Often people do not even know what the problem is, just the headache and everything, especially when you cant raise something, tie up your shoelaces and "so straight your head splits!" - the patients say. This is not stupid, aching pain in the nape, not the throbbing pain of migraine, or the dull eye with cluster pain - this pain is just a bursting. Sometimes you can slightly tap (perepukutirovat) in the projection of the alleged sinusitis and get a completely reasonable response of the patient in response with increased pain.
Types of synogenic facial and headache:
- Frontal (frontal) sinus - pain in the forehead, crown and above / behind the eye.
- The maxillary sinus is a pain in the area of the upper teeth and painters. Often these patients lead dentists, when they check that the teeth are fine.
- Etmoiditis - postorbital pain with irradiation in the temple.
- Sphenoiditis - Temya, forehead, postorbital part, even the occiput.
Treatment - of course, you need to treat not so much a headache as its source. First, we need to take a snapshot of the paranasal sinuses or CT scan, to assess whether it is worthwhile to prescribe antibiotics. Then, the hormones in the nose, regular intensive washing, NSAIDs and watch development. With chronic sinusitis, all sorts of polyps and mucoceles - a separate issue.
Headache in a hangover state
Pain with a hangover - a classic pain of tension + cervicogenic headache. We have natural mechanisms for changing the position of the body in a dream, so as not to "lay" limbs or head. Alcohol turns these mechanisms off and we in what position have fallen, in this and we sleep, sometimes this position is inconvenient for the cervical spine and accordingly leads the neck muscles into hypertonia. You wake up already without alcoholic anesthesia and with combined headaches.
Why is it that on the eve of a dream, before a hangover, you drink analgin and then do not hurt? Well, most likely initially turn off the inflammatory cascade, which then gives pain. Why does not it work then? Most likely because the cascade involves in the heat not only the muscles, but also the nervous structures to which the drugs that you take do not work. Or, in addition to the tension headache, a migraine attack develops, and as I described above, it should be stopped immediately, with time it is more difficult to cope with it.
I myself do not tolerate pain, I take paracetamol 1 g, it is better in a popper like Effergangan, and I drink a lot of liquid. If you feel sick, then the tablet metoclopramide under the tongue and after 5-10 minutes I drink water.
Via zozhnik.ru & wiki


Comments
When commenting on, remember that the content and tone of your message can hurt the feelings of real people, show respect and tolerance to your interlocutors even if you do not share their opinion, your behavior in the conditions of freedom of expression and anonymity provided by the Internet, changes Not only virtual, but also the real world. All comments are hidden from the index, spam is controlled.